| Clin Mol Hepatol > Volume 28(1); 2022 > Article |
|
See the commentary-article "Nonalcoholic fatty liver disease-based risk prediction of adverse pregnancy outcomes: Ready for prime time?" on page 47.
ABSTRACT
Background/Aims
Methods
Results
FOOTNOTES
SUPPLEMENTAL MATERIAL
Supplementary┬ĀTable┬Ā1.
Figure┬Ā1.
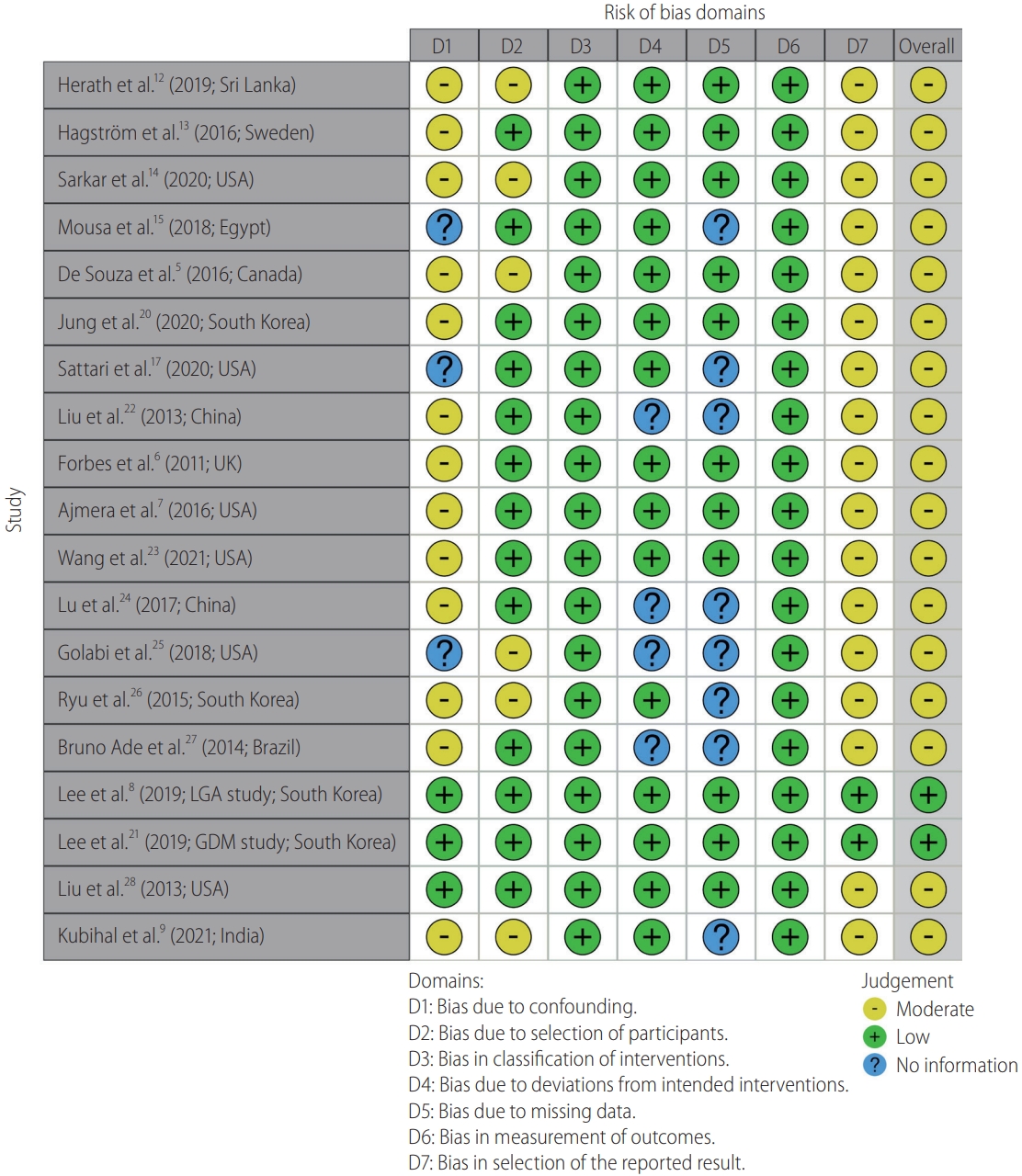
Figure┬Ā3.
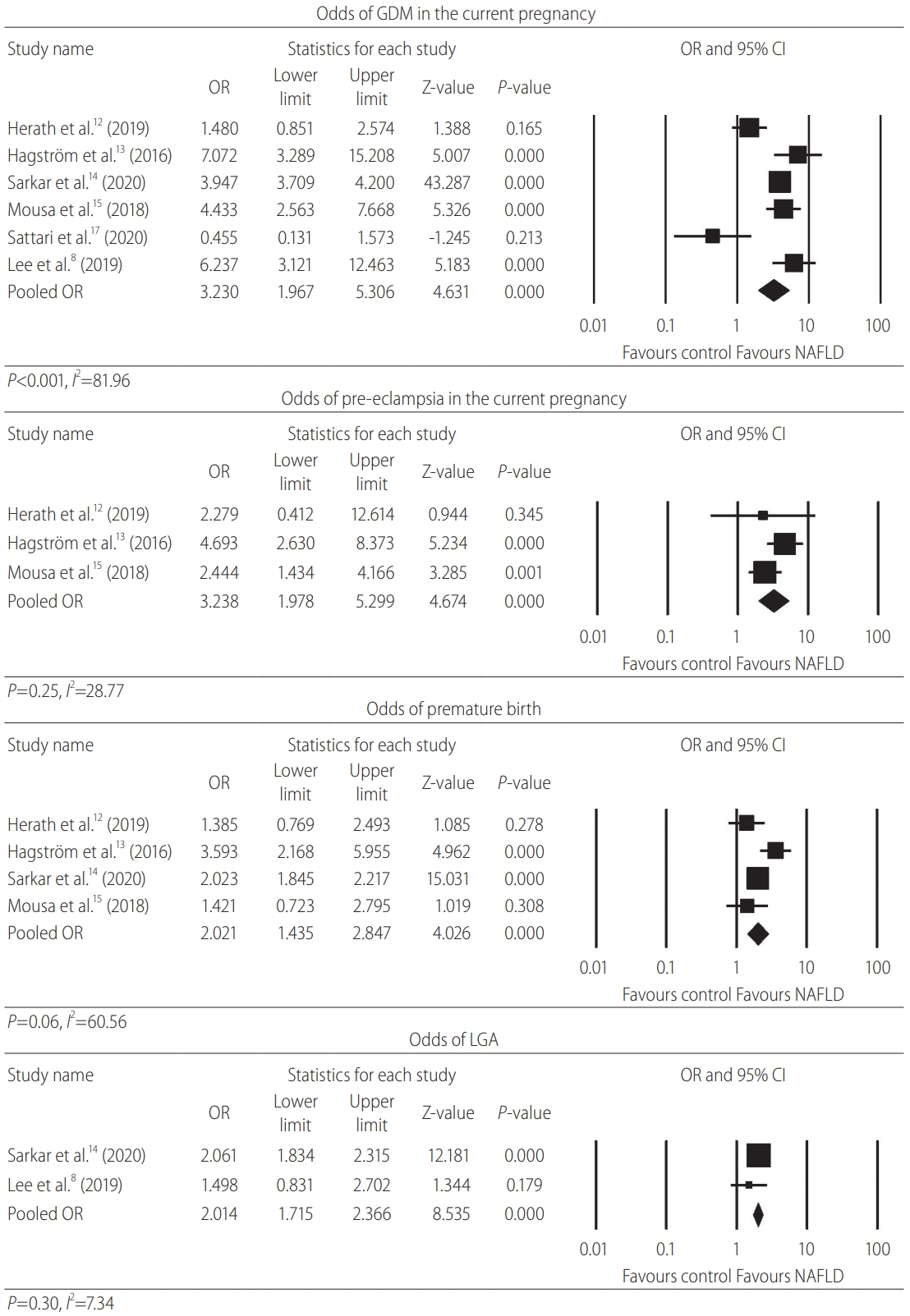
Table┬Ā1.
| Study | Study type | Quality assessment tool | Study score | Total possible score |
|---|---|---|---|---|
| Herath et al. [12] (2019) | Cross-sectional | Newcastle-Ottawa scale* | 8 | 10 |
| Hagstr├Čm et al. [13] (2016) | Cohort study | Newcastle-Ottawa scale | 7 | 9 |
| Sarkar et al. [14] (2020) | Cohort study | Newcastle-Ottawa scale | 8 | 8 (1├Ś question is not applicable) |
| Mousa et al. [15] (2018) | Cohort study | Newcastle-Ottawa scale | 7 | 9 |
| Page et al. [16] (2011) | Case series | MOGA/IHE quality appraisal tool | 10 | 15 (3├Ś question is not applicable) |
| De Souza et al. [5] (2016) | Cohort study | Newcastle-Ottawa scale | 7 | 9 |
| Jung et al. [20] (2020) | Cohort study | Newcastle-Ottawa scale | 7 | 9 |
| Sattari et al. [17] (2020) | Cohort study | Newcastle-Ottawa scale | 6 | 9 |
| Rosenbluth et al. [18] (2020) | Cohort study | Newcastle-Ottawa scale | N/AŌĆĀ | N/AŌĆĀ |
| Ali et al. [19] (2018) | Cohort study | Newcastle-Ottawa scale | N/AŌĆĀ | N/AŌĆĀ |
| Liu et al. [22] (2013) | Cross-sectional | Newcastle-Ottawa scale* | 8 | 9 (1├Ś question is not applicable) |
| Forbes et al. [6] (2011) | Cohort study | Newcastle-Ottawa scale | 8 | 9 |
| Ajmera et al. [7] (2016) | Cohort study | Newcastle-Ottawa scale | 7 | 9 |
| Wang et al. [23] (2021) | Case-control | Newcastle-Ottawa scale | 6 | 9 |
| Lu et al. [24] (2017) | Cross-sectional | Newcastle-Ottawa scale* | 10 | 10 |
| Golabi et al. [25] (2018) | Cross-sectional | Newcastle-Ottawa scale* | 7 | 10 |
| Ryu et al. [26] (2015) | Cohort study | Newcastle-Ottawa scale | 6 | 9 |
| Bruno Ade et al. [27] (2014) | Cross-sectional | Newcastle-Ottawa scale* | 8 | 9 (1├Ś question is not applicable) |
| Lee et al. [8] (2019; LGA study) | Cohort study | Newcastle-Ottawa scale | 6 | 9 |
| Lee et al. [21] (2019; GDM study) | Cohort study | Newcastle-Ottawa scale | 7 | 9 |
| Liu et al. [28] (2013) | Cross-sectional | Newcastle-Ottawa scale* | 8 | 10 |
| Kubihal et al. [9] (2021) | Cross-sectional | Newcastle-Ottawa scale* | 9 | 10 |
Individual study quality assessments, observational studies were assessed using the Newcastle-Ottawa scale whilst case series were assessed by the MOGA/IHE quality appraisal tool.
N/A, not applicable.
Table┬Ā2.
The prevalence was based on the random effects model. Prevalence data of the overall pooled data relating to pregnancy related outcomes in the metaanalysis.
NAFLD, non-alcoholic fatty liver disease; ER, event rate; CI, confidence interval; GDM, gestational diabetes mellitus; DM, diabetes mellitus; GHTN, gestational hypertension; HELLP, haemolysis, elevated liver enzymes, low platelet count; BMI, body mass index; LSCS, low section caesarean section; LGA, large for gestational age birth; IUGR, intrauterine growth restriction; PPH, post-partum haemorrhage; Para 1, second pregnancy; Para Ōēź2, 3rd or later pregnancy; LBW, low birth weight; NASH, non-alcoholic steatohepatitis; NAFL, non alcoholic fatty liver.
Table┬Ā3.
| Study | Exclusion of significant alcohol consumption | Exclusion of other causes of hepatic steatosis | Absence of coexisting chronic liver disease | Demonstration of hepatic steatosis by imaging or biopsy | Satisfied NAFLD Criteria were met |
|---|---|---|---|---|---|
| Herath et al. [12] (2019) | Yes | Yes | Yes | Imaging (USAB) | Yes |
| Hagstr├Čm et al. [13] (2016) | Not reported | Not reported | Not reported | Not reported | Unknown |
| Sarkar et al. [14] (2020) | Not reported | Not reported | Not reported | Not reported | Unknown |
| Mousa et al. [15] (2018) | Yes | Yes | Yes | Imaging (USAB) | Yes |
| Page et al. [16] (2011) | Yes | Yes | Yes | Imaging (4/5 patients) or Histology (1/5 patients) | Yes |
| De Souza et al. [5] (2016) | Yes | Yes | Yes | Imaging (USAB) | Yes |
| Jung et al. [20] (2020) | Yes | No | Yes | Imaging (USAB) | Unknown |
| Sattari et al. [17] (2020) | Not reported | Not reported | Yes | Imaging (USAB) | Unknown |
| Liu et al. [22] (2013) | Yes | Not reported | Yes | Imaging | Unknown |
| Forbes et al. [6] (2011) | Not reported | Not reported | Not reported | Imaging | Unknown |
| Ajmera et al. [7] (2016) | Yes | Yes | Not reported | Imaging (CT scan) | Unknown |
| Wang et al. [23] (2021) | Not reported | Not reported | Not reported | Not reported | Unknown |
| Lu et al. [24] (2017) | Yes | Not reported | Yes | Imaging (USAB) | Unknown |
| Golabi et al. [25] (2018) | Yes | Not reported | Yes | Imaging (USAB) | Unknown |
| Ryu et al. [26] (2015) | Yes | Yes | Yes | Imaging (USAB) | Yes |
| Bruno Ade et al. [27] (2014) | Yes | Yes | Yes | Imaging (USAB) | Yes |
| Lee et al. [8] (2019; LGA study) | Yes | Yes | Yes | Imaging (USAB) | Yes |
| Lee et al. [21] (2019; GDM study) | Yes | Yes | Yes | Imaging (USAB) | Yes |
| Liu et al. [28] (2013) | Yes | Partial | Not reported | Imaging (USAB) | Unknown |
| Kubihal et al. [9] (2021) | Yes | Yes | Yes | Imaging (USAB) | Yes |
Abbreviations
REFERENCES
- TOOLS
-
METRICS

- ORCID iDs
-
Hydar El Jamaly

https://orcid.org/0000-0002-8591-2548 - Related articles
-
The growing burden of non-alcoholic fatty liver disease on mortality2023 April;29(2)
Nonalcoholic fatty liver disease and non-liver comorbidities2023 February;29(Suppl)



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Supplement1
Supplement1 Print
Print



