| Clin Mol Hepatol > Volume 29(Suppl); 2023 > Article |
|
See the commentary-article "Changing the nomenclature from nonalcoholic fatty liver disease to metabolic dysfunction-associated fatty liver disease is more than a change in terminology" on page 371.
ABSTRACT
ŌĆ£Metabolic dysfunction-associated fatty liver disease (MAFLD)ŌĆØ is the term suggested in 2020 to refer to fatty liver disease related to systemic metabolic dysregulation. The name change from nonalcoholic fatty liver disease (NAFLD) to MAFLD comes with a simple set of criteria to enable easy diagnosis at the bedside for the general medical community, including primary care physicians. Since the introduction of the term, there have been key areas in which the superiority of MAFLD over the traditional NAFLD terminology has been demonstrated, including for the risk of liver and extrahepatic mortality, disease associations, and for identifying high-risk individuals. Additionally, MAFLD has been adopted by a number of leading pan-national and national societies due to its concise diagnostic criterion, removal of the requirement to exclude concomitant liver diseases, and reduction in the stigma associated with this condition. The current article explores the differences between MAFLD and NAFLD diagnosis, areas of benefit, some potential limitations, and how the MAFLD terminology has opened up new fields of research.
Excess fat deposition within the liver has been recognized for centuries. In a landmark paper published by Ludwig et al. [1] (1980), the term ŌĆ£non-alcoholic steatohepatitis (NASH)ŌĆØ was first used to describe the liver histology associated with excess liver fat in the absence of significant alcohol consumption. The term ŌĆ£non-alcoholicŌĆØ used by the researchers was derived from similarities in the histopathological findings of these patients compared to those with alcohol-related liver disease, due to the lack of knowledge about its pathophysiological basis at that time [1].
Ever since the introduction of the term nonalcoholic fatty liver disease (NAFLD) into the medical compendium, there has been discussions around changing the name to better reflect the disease process and extending the terminology beyond the superficial histopathological similarities to alcohol-related liver disease [2,3]. In early 2020, an international panel of experts led a consensus-driven process to develop a more appropriate term for the disease. Utilizing a 2-stage Delphi consensus, the term that was proposed was ŌĆ£metabolic dysfunction-associated fatty liver disease,ŌĆØ or ŌĆ£MAFLDŌĆØ [4].
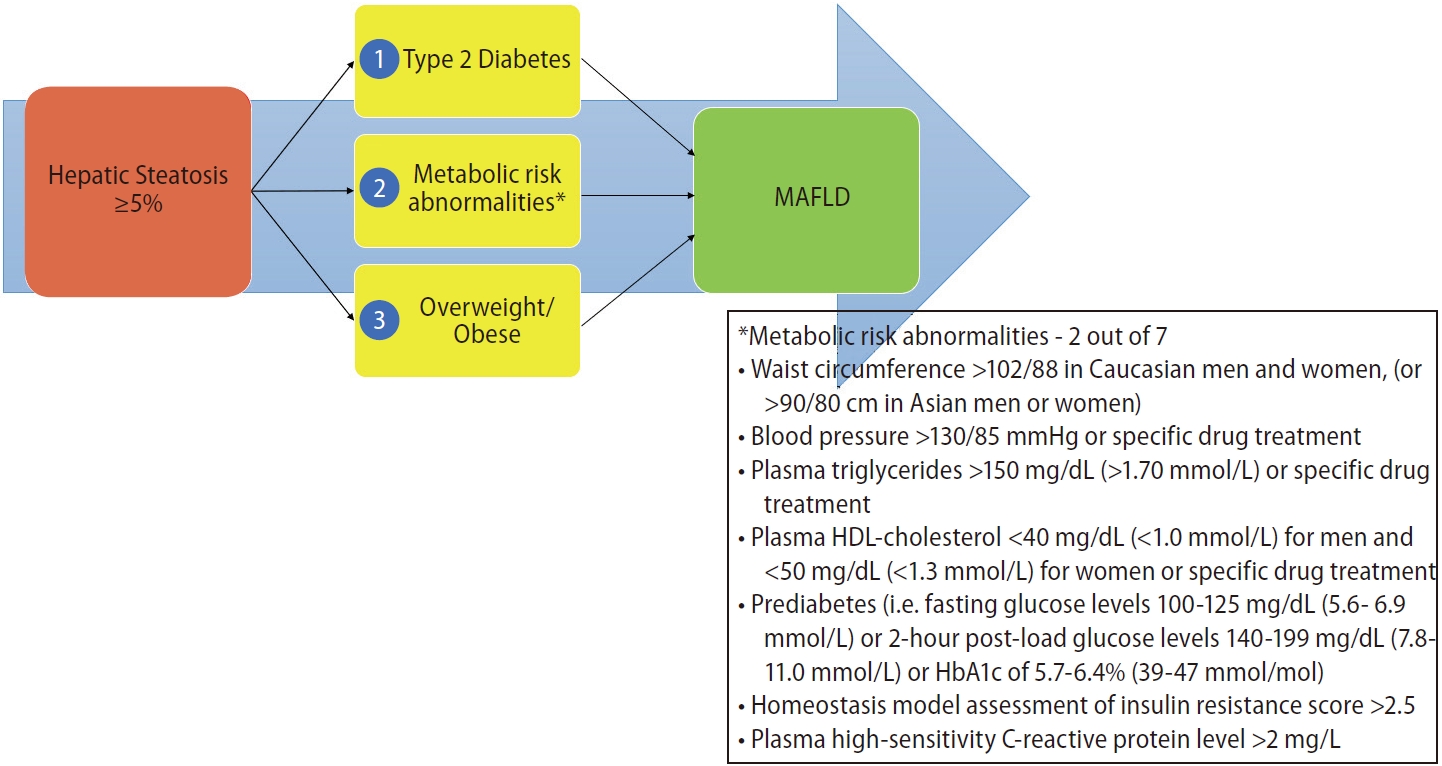
In addition to the name change, the consensus proposed a set of simple positive criteria to diagnose and evaluate individuals for the disease [4]. The diagnostic criterion highlighted the contribution that systemic metabolic dysregulation plays in driving the liver disease (Fig. 1). These contributory factors have since been identified as core research in the field of ŌĆ£NAFLDŌĆØ and its extra-hepatic associations [5].
Since the introduction of MAFLD in 2020 as an alternative term with its own set of diagnostic criteria, there have been more than 800 unique articles referencing the new diagnosis. There has also been controversy with some societies supporting its usage and introducing it as a formal change in terminology and diagnosis in their guidelines [6-10]. This article expands on the differences between MAFLD and NAFLD and the potential benefits and detriments of this change.
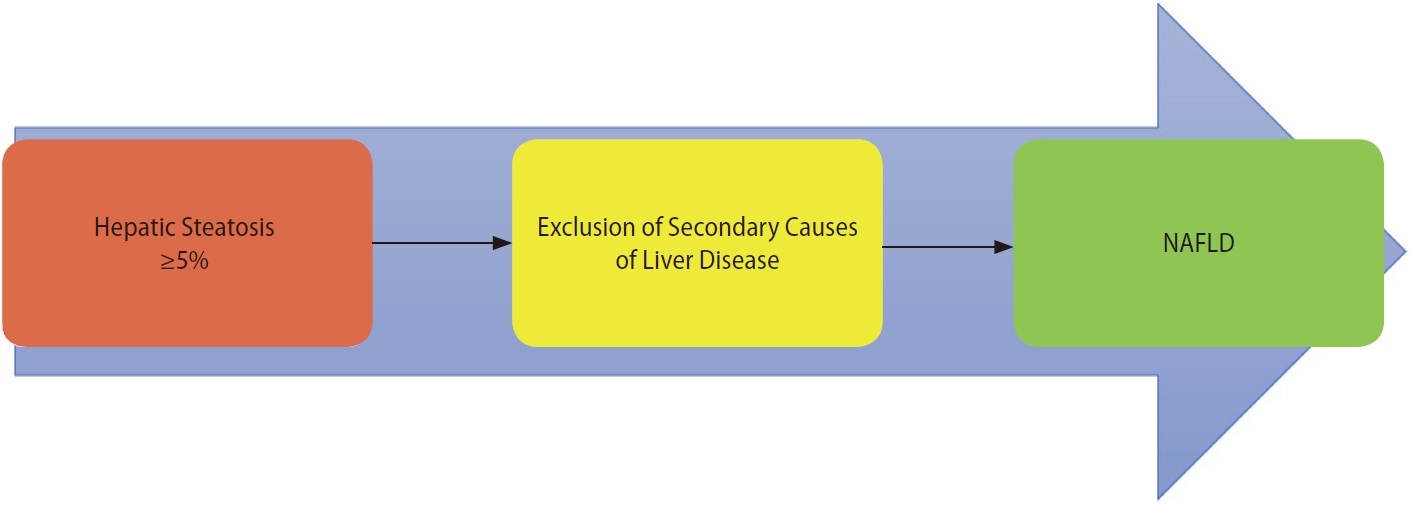
The NAFLD diagnosis, as published in guidelines, requires hepatic steatosis of Ōēź5% without concurrent liver disease, including ŌĆ£significantŌĆØ alcohol usage (Fig. 2) [11]. The criterion for MAFLD utilizes the same standard for hepatic steatosis, but identifies metabolic dysregulatory factors as a pre-requisite for the diagnosis to be entertained (Fig. 1) [4]. The metabolic risk drivers, according to the MAFLD criteria, are type 2 diabetes mellitus and overweight/obesity by ethnicspecific body mass index (BMI) classifications. Both of these risk factors are classically involved in liver fat deposition, and have been noted to be associated with an increase in disease progression and of hepatic and extra-hepatic complications. The third dysregulatory pathway is less commonly recognized but is part of the operational definition of metabolic syndrome. For the diagnosis of MAFLD in healthy weight people, an individual needs to have two of the seven risk factors to make a diagnosis. The risk factors include waist circumference, blood pressure, plasma triglycerides, plasma high-density lipoprotein-cholesterol, prediabetes, homeostasis model assessment of insulin resistance score, and plasma high sensitivity C-reactive protein. The combination of hepatic steatosis with one of these three metabolic risk stratifications results in the diagnosis of MAFLD [4].
The most significant difference between NAFLD and the diagnosis of MAFLD, however, is not the formal recognition of metabolic dysregulatory pathways in the development of the disease, but rather the removal of exclusion of concurrent liver disease to entertain the diagnosis [4,12]. Multiple studies have shown the synergistic effects of comorbid liver disease, including viral hepatitis, and concurrent alcohol usage; however, the exclusion of these in the diagnosis of NAFLD underpins a cognitive dissonance between these disease processes, attempting to exclude their contribution to individualized patient outcomes [13,14]. In short, MAFLD tells us what the disease is and not what it is not, and MAFLD is unrelated to the presence or absence of other causes of liver disease. This simple change has allowed clinicians to identify and treat all the liver diseases that might exist in a given patient in a holistic manner. The latter is important, given that in many countries and regions, overweight or obesity impacts over 60% of the adult population.
The switch to a set of positive diagnostic criteria results in the ability to detect all underlying liver diseases, particularly in patients without apparently clear metabolic features. A recent study by Alexander et al. [15] (2018) utilized multiple European primary care databases to determine the prevalence of NAFLD in general practice among 17.7 million patients. It found that the pooled prevalence of NAFLD was significantly lower than expected, with only 1.9% given this diagnosis in 2015 compared to prior observational studies estimating a prevalence of 20ŌĆō30% in the European population. Although the prevalence has doubled since 2007 in these general practice databases, their recognition has not increased to meet the conservative estimates of this disorder.
In the age of improved investigations, there has been a significant move in most specialties to create positive diagnostic criterion for diseases. The benefits include decreased time to diagnosis and initiation of treatment, as well as consistent diagnosis facilitating both collaboration and research into the underlying disorders [4,16]. While this has occurred in a number of specialties, the prevalence of these disorders has been rare, and has not garnered the level of controversy that the proposed terminology of MAFLD has within the liver community. A recent example is the change from primary biliary cirrhosis to primary biliary cholangitis, which better reflects the pathophysiological manifestations of the disease process, as this condition has rarely resulted in cirrhosis.
For a disorder with a significant prevalence in the community, the NAFLD diagnostic criteria did not lead to increased understanding in the healthcare community and the wider general public. Fatty liver deposition is one of the most prevalent conditions affecting up to 40% of the general population; however, the recognition of the condition and its associated complications is poor [17]. One of the major controversies regarding the change in terminology to MAFLD is the suggestion that a name change will impair the current work to improve public awareness of NAFLD. However, the public awareness of NAFLD as a condition of concern is surprisingly low (around 4%), despite being included in the medical compendium for over 40 years [17]. There have been some suggestions that the change in name from NAFLD to MAFLD will increase public awareness of this condition [16,18,19].
MAFLD diagnosis has been crucial in identifying higher-risk patients who would benefit from targeted management. Several studies have highlighted that a MAFLD diagnosis better correlates with higher liver fibrosis stage and non-invasive markers of fatty infiltration [20-23]. This recognition that metabolic dysregulatory pathways contribute to more significant liver disease highlights the important difference of the MAFLD diagnostic criteria over the NAFLD exclusionary criteria to assess individuals suffering from the disease.
Despite the histopathological premise for the term NAFLD and advances in understanding the pathophysiological basis of the disease with many patient and healthcare suggestions for a name change, no new terminology has been developed and NAFLD has subsisted in the literature for decades [24]. Moreover, utilization of the diagnosis of NAFLD in healthcare outside of the gastroenterology specialty has been sparse. In a survey conducted by non-gastroenterology specialists in Australia, 56% of the respondents believed that NAFLD was related to alcohol intake [25]. This suggests that, despite non-alcoholic being the defining feature of the term ŌĆ£NAFLDŌĆØ documented clearly within the name, the term is nebulous even among hospital specialists and not reflective of the practice need.
Another key characteristic of NAFLD is the exclusion of harmful alcohol intake in individuals with the disease. There are a number of reasons why harmful alcohol intake should not be used as an exclusionary tool in fatty liver disease. The first is that alcohol intake is a self-reported measure by a patient and has a variable designation of volume in different societal settings. Due to the stigma associated with alcohol consumption and its effects on the liver, under-reporting by patients has been identified [26]. A recent study performed by Staufer et al. [27] in 2022 also has also called into question the utilization of NAFLD after examining ethyl glucuronide in hair samples collected to assess alcohol consumption. In this prospective study, 114 patients were diagnosed with NAFLD after exclusion of other chronic liver diseases and alcohol consumption by patient recall. Harmful alcohol consumption was designated as >20 g of EtOH/day for women and >30 g of EtOH/day for men. The study found that 29% of the patients diagnosed with NAFLD had high to moderate risk of alcohol-related liver damage with repeated moderate to excessive alcohol consumption after being confronted with hair analysis, showing elevated levels of ethyl glucuronide. In a study directly assessing NAFLD diagnosis, almost 30% of the patients had elevated alcohol levels, which contradicted the basis for the diagnosis of NAFLD [27].
Confounding the picture even further is a recent paper by Meijnikman et al. [28] (2022) regarding the role of the gut microbiome in generating endogenous ethanol. In that study assessing obese NAFLD and NASH patients, portal vein and peripheral blood were taken to assess ethanol. It showed that microbiome-related ethanol production occurs in all populations, but was significantly higher in NASH and NAFLD when compared to patients without hepatic steatosis. This microbiome-induced ethanol production did not produce high peripheral concentrations of alcohol due to the liversŌĆÖ ability to process large quantities of ethanol. The main point of this study was that, even though exogenous ethanol has been accounted for in the diagnostic terminology, there is a possibility that endogenous ethanol production by the microbiome could be contributory to its development [28]. Due to the histopathological similarities between alcohol-related liver disease and NAFLD, it is possible that the mechanism of injury is similar, but from different sources.
Secondly, there is heterogeneous reporting requirements across geographic regions governing the volume of alcohol considered to be harmful. Examples of this include the American Associated for the Study of Liver Disease and the Asian Pacific Association for the Study of the Liver guidelines, which define heavy or at-risk drinking as more than 14 drinks per week for men or more than seven drinks per week for women [11]. In the European Associated for the Study of the Liver guidelines, the diagnosis of NAFLD requires the exclusion of daily alcohol consumption of >30 g for men and >20 g for women [29]. Thirdly, even light or moderate alcohol consumption in the setting of NAFLD, which does not meet the exclusionary criteria set above, can cause significant worsening of fibrosis when compared to no consumption [30]. This has been shown in studies where even mild alcohol usage worsened fibrosis and may synergistically cause cirrhosis in patients diagnosed with NAFLD.
Due to the lack of histological characteristic features distinguishing alcohol-related fatty infiltration from non-alcohol-related fatty liver infiltration, the utilization of ŌĆ£non-alcoholicŌĆØ via comprehensive alcohol assessment as a patient-reported measure with the associated stigmatization calls into question its ongoing use. This is particularly important, as international guidelines have recommended that ŌĆ£non-harmfulŌĆØ alcohol consumption has been shown to worsen fibrosis in patients with fatty liver disease. Additionally, evidence pointing towards increased endogenous ethanol production by the microbiome in fatty liver disease could be contributory to the underlying pathogenesis.
The utilization of previously collected databases to assess the applicability of MAFLD has been undertaken by several authors. The first of these studies performed by Lin et al. used the National Health and Nutrition Examination Surveys (NHANES) from 1988ŌĆō1994, which examined 13,083 patients with complete ultrasonography and laboratory data [31]. Patients who met the MAFLD diagnostic criteria had statistically significant increases in metabolic comorbidities, liver enzymes, and non-invasive liver fibrosis scores compared to the NAFLD group.
A review performed by Kang et al. [32] in 2021 on behalf of the Korean NAFLD study group examined the publications that compared MAFLD to NAFLD, with a particular focus on the combined associations of risks in retrospective studies. It showed that MAFLD had statistically significant increases in alanine transferase (23.96┬▒22.22 vs. 22.31┬▒21.34, PŌēż0.001), NAFLD fibrosis score (ŌĆō2.05┬▒1.51 vs. ŌĆō2.18┬▒1.52, PŌēż0.001), and fibrosis-4 (FIB-4) scores (1.06┬▒1.35 vs. 1.01┬▒0.84, PŌēż0.001) compared to NAFLD. This indicates that MAFLD more specifically selects patients with worse liver function and non-invasive scores. These differences were even more striking in the comparison of MAFLD to non-metabolic risk (MR) NAFLD (or NAFLD patients without the necessary metabolic risk factors to meet the criteria for MAFLD). Utilizing MAFLD diagnostic criteria compared to non-MR NAFLD, the increases became more marked in alanine transferase (23.96┬▒22.22 vs. 16.81┬▒17.84, PŌēż0.001), NAFLD fibrosis score (ŌĆō2.05┬▒1.51 vs. ŌĆō3.00┬▒1.32, PŌēż0.001), and FIB-4 scores (1.06┬▒1.35 vs. 0.87┬▒1.05, PŌēż0.001). This highlights the utility of the MAFLD criteria over the traditional NAFLD diagnostic criteria in assessing patients for worsening liver disease. These analyses of large patient cohorts have also correctly identified most patients who have higher related risks for comorbidities and increased mortality. For example, the diagnosis of MAFLD has been shown to be superior in identifying patients who are most at risk for clinical disease progression compared to NAFLD [21,33].
There is limited historical evidence for the recognition of NAFLD and its contributory factors in the literature. Evidence that is available suggests that NAFLD recognition and diagnosis in primary care settings that manage the majority of patients are poorly understood and applied [15,25,31,34,35]. The simple criteria for MAFLD have been purported to increase the recognition and understanding outside of gastroenterology and hepatology specialists, and it will also enable primary care practitioners and others to initiate early management [16,18,19,36]. This has not been studied in the literature to date, but would be significant to public health as early interventions, similar to cardiovascular disease and diabetes mellitus, are more likely to be efficacious in preventing adverse outcomes.
From an individual patient perspective, the utilization of the term NAFLD has led to many patients trivializing their condition. Several studies have reported that up to 95% of patients with suspected NAFLD are unaware of having liver disease, and that >75% do not feel they are at risk of developing NAFLD [34,35,37]. This minimization of potential harms does a disservice to the prevalence and potential severity of the disease, creating a lack of engagement among patient populations who suffer from NAFLD. Evidence suggests that trivialization mainly arises through an inappropriate name of the condition, or when disease perceptions or diagnoses are confusing to people. Expert opinion governing this area of terminology believe that the negative prefix ŌĆ£non-ŌĆØ carries a perception that the disease is unimportant [16].
One of the particularly onerous societal burdens of NAFLD is the utilization of alcohol in its name. Alcohol usage carries with it a significant stigma, and that stigma has overlapped into the diagnosis of NAFLD [16]. This is particularly damaging in discussing the disease with pediatric patients and practicing Muslim patients, where stigma may prohibit practitioners from discussing the disease with the patients. Recent correspondence regarding the change in terminologiesŌĆÖ impact on the Arab world, with the largest practicing Muslim population, has highlighted the benefit of changing the name to MAFLD [10,38].
Stigmatization of healthcare conditions carries a significant burden. Stigma has negative effects on self-esteem and can lead to decreased self-management of the condition, decreased quality of life, and increased inability to cope with a disease [16]. Stigma can also induce fear in patients, which can lead to adverse health behaviours, including denial of diagnosis, treatment avoidance, lack of compliance with treatment and healthcare advice, and ultimately, termination of treatment [16]. Therefore, stigma should be avoided with any diagnosis label to increase the patientsŌĆÖ motivation to manage their condition and to seek ongoing treatment.
One of the benefits of utilizing MAFLD compared to NAFLD is the increase in the identification of individuals with high-risk features for progressive liver disease. In a study by Ayada et al. [39] (2021), 17 studies containing both a diagnosis of NAFLD and MAFLD comprising 9,808,677 individuals were reviewed. This study showed that the prevalence of MAFLD was 33.0% (95% CI 29.7ŌĆō36.5), with a NAFLD prevalence of 29.1% (95% CI 27.1ŌĆō31.1). The surprising detail of this study was that of all the fatty liver identified in the combined studies, 15.1% were identified with MAFLD-only diagnosis (95% CI 11.5ŌĆō19.5). Several of the studies showed that large increases in the patients diagnosed were undertaken in Asian populations. This indicates that the new diagnostic criteria is better suited to identify patients over the traditional NAFLD diagnosis label [39]. Whilst this has been replicated in other reports, there are geographic variations to this increase in the identification of significant fatty liver disease.
One of the potential detractions from utilizing MAFLD exists in the patients who fulfill the criteria for NAFLD without metabolic risk factors or other identifiable aetiologies of liver disease. When examining retrospective data comparing the two diagnoses, the majority of patients fulfill both the MAFLD and NAFLD criteria. However, there is a small proportion of patients who make up the non-MR NAFLD group across these studies, ranging from 0.6ŌĆō16.1%, with most consistently estimating this group to make up around 5% of the fatty liver disease population [20,22,32,33,40-43]. While most risks were associated with MAFLD diagnosis, some studies did show that non-MR NAFLD patients had increased risks of cardiovascular disease during follow-up, though the majority of studies showed no increase in liver-related risk compared to the control populations [39]. The presence of severe hepatic steatosis has been shown to have implications on metabolic complications, including metabolic syndrome, and thus, these patients should be monitored for the development of complications, especially since metabolic risk factors, including weight and dysglycemia, can increase over time.
Whilst a number of articles have been published on MAFLD vs. NAFLD, there have been numerous negative articles suggesting that MAFLD does not contribute to mortality (Table 1) [14,44-48]. The main point suggested by these articles is that the metabolic dysregulatory features are the cause for mortality, and not the underlying MAFLD diagnosis. This has been shown using adjusted modelling considering type 2 diabetes mellitus and BMI, which were treated as confounders of the demonstrated association that MAFLD displays with mortality. However, there are two major concerns that these articles fail to acknowledge. First, as the diagnosis of MAFLD relies on metabolic dysregulation, type 2 diabetes mellitus and BMI cannot be treated as confoundersŌĆöthey are an integral part of the diagnosis. Put simply, without metabolic dysregulatory changes, there is no MAFLD; therefore, their inclusion as confounders in these adjustment models revokes the diagnosis of MAFLD. These adjustment models only assess fatty liver without a metabolic component, which is hepatic steatosis.
The second point that adjustment modelling indicates is that MAFLD without metabolic derangements does not have any association with mortality. While this has been highlighted to show that the MAFLD diagnosis is ŌĆ£wrongŌĆØ and is then discussed at length, the opposite has been unwittingly demonstrated. What each of these articles has failed to recognize is that adjustment models show that the utilization of metabolic dysregulatory factors is the key cause of increased mortality in fatty liver deposition. Without further metabolic dysregulation, fatty liver per se poses no threat of increased mortality. As metabolic dysregulation is required for the diagnosis of MAFLD, in sum, these articles show that the consensus group was correct in selecting these factors to underpin the major causative pathways that lead to increased mortality.
A study by Moon et al. [44] (2022) assessed individuals from two community-based cohorts, between the ages of 40 and 70 years, and prospectively followed them for a median of 15.7 years. Using the diagnostic criterion for MAFLD and NAFLD and adjusting for confounders, they showed that MAFLD independently predicted the overall mortality with a hazard ratio (HR) 1.33 (95% CI 1.05ŌĆō1.69), while NAFLD was not associated with the overall mortality with a HR of 1.20 (95% CI 0.94ŌĆō1.53). MAFLD also predicted cardiovascular disease after adjustment for age, sex, and BMI, but lost its significance when adjusted for other metabolic dysfunction risk factors, most notably type 2 diabetes mellitus. The latter is not surprising, as discussed earlier, and since these risk factors are more proximal to adverse organ-specific outcomes (e.g., hypertension or atherogenic dyslipidemia for cardiovascular disease).
In utilization of the MAFLD criteria, there is an understanding of the individual phenotypic profiles of the patient that has contributed to the development of fatty liver infiltration [4]. These risks not only provide clues to the causation of fatty liver, but also on the possible treatment and management options. This is important when we address each of the individual phenotypes separately, but also when we note the synergistic effects that each pathway provides for the overall patient outcomes. In contrast, with the diagnosis of NAFLD, a one-size-f its-all approach governs the phenotypic presentation and management.
An example is the risk of type 2 diabetes mellitus in overweight or obese patients. It has been shown that being overweight or obese significantly increases the risks for developing type 2 diabetes mellitus [49]. The underlying mechanisms have not been fully established; however, weight loss in these individuals can ameliorate or even normalize the risk of type 2 diabetes mellitus. Targeted weight loss should be the first step in reducing the risk of developing type 2 diabetes mellitus in overweight or obese patients by decreasing peripheral and hepatic insulin resistance [49]; whereas, in patients with type 2 diabetes mellitus, the first step in management is the normalization of blood sugars. Whilst this can be targeted by weight loss, the specific goal is the normalization of blood sugars. This highlights the contributory metabolic risk factors in the development of further metabolic co-morbidities. Each needs a tailored response to address the underlying needs, despite the interrelated effects of each.
Of note, there have been recent studies demonstrating that a MAFLD diagnosis is associated, on multivariate analysis, with an increased risk of type 2 diabetes mellitus in patients whose metabolic phenotype at diagnosis does not include type 2 diabetes mellitus, compared to a NAFLD diagnosis [50]. This is significant as it demonstrates the early diagnosis of MAFLD over that of NAFLD, which can help target individuals at risk of developing other significant complications, such as type 2 diabetes mellitus. It, therefore, allows clinicians to appropriately target patient populations to modify their metabolic risk profile to prevent complications [50].
Utilizing the definition of MAFLD also highlights the importance of holistic patient management [4]. Currently, the mainstay of initial management of all metabolic disorders is dietary change and exercise. Targeting them holistically, rather than in an organ-specific manner, can lead to widespread improvements in outcomes, particularly with regard to cardiovascular health and cancer, which are the greatest causes of adverse outcomes in fatty liver disease [5]. This is also particularly important for clinical research which focuses on metabolic dysregulation to improve both liver and systemic outcomes.
Outside of the traditional metabolic dysregulatory environments that are included in the diagnostic algorithm for MAFLD, there have been studies that showed an association between MAFLD and other disease processes [51,52].
This is to be expected when placing MAFLD in alignment with other metabolic dysregulation-associated disorders, such as cardiovascular disease, rather than the stand-alone disease entity of NAFLD (Table 2). While cardiovascular disease is the major mortality burden in fatty liver disease, other disorders associated with MAFLD include peripheral vascular disease, chronic kidney disease, and some cancers, especially of the gastrointestinal tract [5].
There have been studies assessing the cardiovascular risk association of MAFLD vs. NAFLD. A study by Lee et al. [53] (2021) evaluated incident cardiovascular disease risk from a nationwide health screening database involving 9,584,399 participants followed for a median of 10.1 years. Patients were placed in fatty liver disease (FLD), NAFLD-only, MAFLD-only, or both FLD groups. Cardiovascular risk was elevated in all fatty liver disease; however, NAFLD-only group had significantly decreased hazard ratio (HR 1.09, 95% CI 1.03ŌĆō1.15) compared to MAFLD-only (HR 1.43, 95% CI 1.41ŌĆō1.43) and both FLD groups (HR 1.56, 95% CI 1.54ŌĆō1.58).
Recent studies assessing NAFLD vs. MAFLD have identified that asymptomatic atherosclerotic cardiovascular disease has an independent association on multivariable logistic regression models with MAFLD, but not with NAFLD diagnosis [54]. This is significant due to the burden of cardiovascular disease in patients suffering from fatty liver infiltration. Therefore, MAFLD diagnosis assists in identifying patients who should undergo cardiovascular assessment and intervention over the traditional NAFLD diagnosis.
Other associations made with NAFLD have been assessed against the MAFLD criteria to assess the strength of the associations with the change in terminology. A study by Sun et al. [49] (2021) utilized the NHANES database to assess the correlation of MAFLD with chronic kidney disease (CKD) and abnormal albuminuria. In that study, MAFLD patients had a lower estimated glomerular filtration rate (74.96┬▒18.21 vs. 76.46┬▒18.24 mL/min/1.73m2, P<0.001) and a greater prevalence of CKD (29.60% vs. 26.56%, P<0.005) compared to those with NAFLD.
Studies addressing the association between MAFLD and other conditions are currently underway. While several conditions, such as breast lesions, have shown that MAFLD is related with these conditions, similar to NAFLD, no direct comparison has been published. It would be interesting to note the strength of association of the conditions that were previously noted to be associated with NAFLD, as well as the impact of the MAFLD criteria on them.
Somewhat surprisingly, MAFLD has shown associations with lung conditions over a NAFLD diagnosis, with poorer lung function and higher rates of mortality associated with COVID19 infection. A study performed by Miao et al. [56] (2022) compared the association of lung function parameters in patients diagnosed with MAFLD vs. NAFLD. After adjusting for age, sex, adiposity measures, smoking status, and alcohol intake, MAFLD subjects had significantly lower predicted forced vital capacity (88.27┬▒17.60% vs. 90.82┬▒16.85%, P<0.005) and lower 1 second forced expiratory volume (FEV1) (79.89┬▒17.34 vs. 83.02┬▒16.66%, P<0.005) when compared to those diagnosed with NAFLD. While the results suggest that MAFLD has a greater role in identifying patients with reduced lung function, it is likely related to MAFLD selecting patients with higher non-invasive liver fibrosis scores. Every 1-point increase in FIB-4 resulted in a decrease in FVC by 0.507 (95% CI ŌĆō0.840 to ŌĆō0.173, P=0.003) and a decrease in FEV1 by 0.439 (95% CI ŌĆō0.739 to ŌĆō0.140, P=0.004).
The additive basis of MAFLD with other liver diseases is a main advantage over the traditional NAFLD definition. Since NAFLD excludes concomitant liver diseases, such as hepatitis B or C, there was no ability for the patients to have dual etiologies for their liver disease. Substantive literature has shown that individuals who have underlying liver diseases from hepatitis B and hepatitis C, with a diagnosis of MAFLD, have significantly increased complications, both intra- and extra-hepatic [13]. The additional diagnosis of MAFLD coupled with hepatitis B, for example, increases the rates of complications and mortality [57].
In a recent study by Zheng et al. [58], among 780 patients with liver biopsies, 773 were given a diagnosis of MAFLD. Of the patients with MAFLD, 66 also had excess alcohol consumption. On subgroup analysis assessing MAFLD patients with significant alcohol consumption, the patients had high gamma-glutamyl transferase levels and exhibited more hepatic steatosis when compared to patients with MAFLD without co-existing liver disease. This outcome could not be evaluated in previous studies with NAFLD due to the requirement to exclude co-existing liver disease.
Due to the restrictive nature of NAFLD not allowing concurrent liver disease as a requirement for diagnosis, treatment strategies have focused on single liver disease entities [11]. With the more finessed MAFLD diagnosis, the co-existence of separate entities of liver disease can be entertained [4]. This allows clinicians to manage one or more conditions simultaneously, rather than treating a ŌĆ£dominantŌĆØ liver disease.
While there is currently no approved medical treatment for MAFLD, there are a number of phase III trials underway that are showing promising preliminary results [59]. One of the major benefits of a MAFLD diagnosis, which has been overlooked in the debate over terminology, is the potential inability to provide treatment for fatty liver infiltration in individuals with concurrent liver pathologies [4,7]. This underscores the most serious implication of the NAFLD terminology in excluding significant proportions of the population who would benefit from future treatments.
The inclusion for NAFLD clinical studies has been based on a hepatic phenotype in the absence of significant alcohol intake and all concurrent steatosis-associated liver pathologies. The move forward with MAFLD proposes that the basis for intervention should focus on the pathogenic drivers. This change will move research on fatty liver from a ŌĆ£one-size-fits-allŌĆØ situation to a more nuanced treatment of its pathophysiological determinants [36].
Previous correspondence has suggested that the name change to MAFLD may hinder the interpretation of studies that are currently ongoing [60]. The major concern is regarding the utilization of ŌĆ£resolution of NASH with no worsening of liver fibrosis,ŌĆØ which is a key histological endpoint for conditional drug approval [61]. Negating this argument, the MAFLD criteria do not propose any change in pathological criteria for a diagnosis of metabolic steatohepatitis.
When selecting patients for fatty liver disease trials, there is confounding bias associated with the NAFLD terminology [62]. Whilst the exclusionary criteria of alcohol and other contributory liver diseases are standard, there is no mechanism to explore the pathogenic aspects of the underlying liver fat infiltration. We have already discussed concerns with alcohol usage in patients with NAFLD with significant underestimation likely in clinical practice. With the utilization of MAFLD and the strict criteria for assessing metabolic co-factors, however, clinical trials inclusion will identify a more homogenous group of patients.
While the controversy regarding NAFLD vs. MAFLD is ongoing, the debate is also polarizing. Although MAFLD will not capture every single patient, it does capture those who require early intervention and are at increased risk of disease progression. Therefore, in our perspective, it would on balance be more beneficial to further develop the MAFLD concept for improved patient care and clinical research (Table 3).
There are significant clinical, research, and patient benefits to the utilization of MAFLD over the NAFLD terminology. MAFLD establishes a clear diagnosis due to a set of positive diagnostic criteria that allows clinicians to better tailor practice to target individuals at high risk of developing complications or other metabolic co-morbidities. Therefore, we contend that the term ŌĆ£MAFLDŌĆØ is a step in the right direction to decrease the stigma associated with a NAFLD diagnosis, to increase public awareness and to improve clinical care.
FOOTNOTES
Figure┬Ā1.
Diagnostic criterion for MAFLD. MAFLD, metabolic dysfunction-associated fatty liver disease; HDL, high-density lipoprotein.
Table┬Ā1.
Mortality difference between MAFLD and NAFLD
| Study | Patients (n) | Outcomes |
|---|---|---|
| Huang et al. [45] (2021) | Total/MAFLD/NAFLD=4,437/3,909/3,779 | 1. MAFLD increased overall mortality compared to NAFLD (HR 2.07 vs. 1.47) ŌĆō difference was non-significant after adjusting for metabolic parameters. |
| Both MAFLD and NAFLD=3,251 | ||
| NHANES III | MAFLD only=658 | 2. NAFLD-only had reduced total mortality (HR 0.46, 95% CI 0.24ŌĆō0.89). |
| NAFLD only=528 | . | |
| Muthiah et al. [46] (2022) | Total/MAFLD/NAFLD=4,982/4,982/excluded | MAFLD-only had increased overall all-cause mortality compared to MAFLD+NAFLD (HR 1.27, 95% CI 1.11ŌĆō1.48). |
| Both MAFLD and NAFLD=2,950 | ||
| NHANES III ŌĆō Type 2 diabetes patients | MAFLD only=2,032 | |
| NAFLD only= Excluded | ||
| Younossi et al. [14] (2022) | Total/MAFLD/NAFLD=2,617/2,332/2,122 | 1. Study excluded all patients with viral hepatitis. |
| Both MAFLD and NAFLD=1,915 | 2. MAFLD-only had significantly increased all-cause mortality when compared to MAFLD+NAFLD (HR 2.28, 95% CI 1.84ŌĆō2.82, P<0.001 vs. 1.89, 95% CI 1.68ŌĆō2.11, P<0.001). | |
| NHANES III+NHANES 2017ŌĆō2018 participants | MAFLD only=418 | |
| NAFLD only=207 | 3. NAFLD-only had a protective effect on all-cause mortality (HR 0.57, 95% CI 0.34ŌĆō0.96, P=0.0335). | |
| Fatty liver disease not defined by MAFLD or NAFLD=78 | 4. When adjusted for age, sex, race, education, income, marital status, smoking status, healthy eating index, BMI, physical activity, and alcohol-related liver disease, only MAFLD+NAFLD had increased all-cause mortality (HR 1.15, 95% CI 1.04ŌĆō1.28, P=0.0091). | |
| Nguyen et al. [47] (2021) | Total/MAFLD/NAFLD=2,997/2,742/2,494 | 1. On unadjusted modelling MAFLD-only had higher increased overall mortality compared to NAFLD+MAFLD (HR 4.6, 95% CI 2.6ŌĆō7.9, P<0.001 vs. 3.2, 95% CI 2.0ŌĆō5.2, P<0.001). On adjusted modelling, MAFLD-only was associated with increased mortality (HR 2.4, 95% CI 1.2ŌĆō4.6, P=0.01). |
| NHANES III | Both MAFLD and NAFLD=2,240 | |
| MAFLD only=503 | 2. On unadjusted modelling, MAFLD-only had higher increased cancer related mortality vs. NAFLD+MAFLD (HR 3.9, 95% CI 1.7ŌĆō8.9, P=0.002 vs 2.7, 95% CI 1.2ŌĆō6.0, P=0.02). On adjusted modelling, neither MAFLD only nor NAFLD+MAFLD had statistically significant association with cancer-related mortality. | |
| NAFLD only=254 | 3. On unadjusted modelling, MAFLD-only had higher increased other cause mortality vs. NAFLD+MAFLD (HR 4.0, 95% CI 2.1ŌĆō7.6, P=<0.001 vs. 2.8, 95% CI 1.5ŌĆō5.2, P=0.002). On adjusted modelling, neither MAFLD-only nor NAFLD+MAFLD had statistically significant associations with other cause mortality. | |
| Semmler et al. [48] (2021) | Total/MAFLD/NAFLD=4,718/2,189/2,262 | 1. Increased mortality was observed in lean MAFLD compared to lean NAFLD and no hepatic steatosis (8.6% vs. 2.7% vs. 5.6%). |
| SAKKOPI database | Both MAFLD and NAFLD | 2. Increased mortality was observed in overweight MAFLD compared to overweight without hepatic steatosis (6.8% vs. 3.7%). |
| MAFLD only | 3. Increased mortality was observed in obese MAFLD compared to obese without hepatic steatosis (7.1% vs. 6.5%). | |
| NAFLD only=73 | 4. On adjusted modelling with age and components of metabolic syndrome, MAFLD was not associated with increased mortality (HR 1.115, 95% CI 0.822ŌĆō1.512, P=0.484). |
Table┬Ā2.
Cardiovascular mortality difference between MAFLD and NAFLD
| Study | Patients (n) | Outcomes |
|---|---|---|
| Muthiah et al. [46] (2022) | Total/MAFLD/NAFLD=4,982/4,982/excluded | 1. MAFLD-only had increased cardiovascular mortality compared to MAFLD+NAFLD (HR 1.26, 95% CI 1.05ŌĆō1.52). |
| NHANES III ŌĆō Type 2 diabetes patients | Both MAFLD and NAFLD=2,950 | |
| MAFLD only=2,032 | ||
| NAFLD only=Excluded | ||
| Niriella et al. [51] 2021 | Total/MAFLD/NAFLD=2,985/990/940 | 1. MAFLD had increased overall cardiovascular non-fatal and fatal events when compared to NAFLD (RR 4.2, 95% CI 1.5ŌĆō11.5 vs. RR 3.7, 95% CI 1.3ŌĆō10.3, P<0.006). |
| Community-based cohort study with 7-year follow-up | Both MAFLD and NAFLD=902 | |
| MAFLD only=88 | 2. MAFLD-only had significantly higher rates of cardiovascular non-fatal and fatal events when compared to NAFLD only (RR 7.2, 95% CI 2.4ŌĆō21.5 vs. RR 1.9, 95% CI 0.25ŌĆō14.8). | |
| NAFLD only=38 | ||
| Nguyen et al. [47] (2021) | Total/MAFLD/NAFLD=2,997/2,742/2,494 | 1. On unadjusted modelling, MAFLD-only had higher increased cardiovascular disease mortality vs. NAFLD+MAFLD (HR 9.4, 95% CI 2.6ŌĆō34.6, P=0.001 vs. HR 7.0, 95% CI |
| NHANES III | Both MAFLD and NAFLD=2,240 | |
| MAFLD only=503 | 2.1ŌĆō23.1, P=0.002). On adjusted modelling, neither MAFLD-only or NAFLD+MAFLD had statistically significant associations with cardiovascular mortality, but MAFLD-only had a trend towards significance (HR 6.7, 95% CI 0.9ŌĆō47.1, P=0.06). | |
| NAFLD only=254 | ||
| Lee et al. [53] (2021) | Total/MAFLD/NAFLD=3,628,540/2,680,217/3,573,644 | 1. NAFLD+MAFLD had higher increased cardiovascular events when compared to MAFLD-only and NAFLD-only (HR 1.56, 95%CI 1.54ŌĆō1.58 vs. HR 1.43, 95% CI 1.41ŌĆō1.45 vs. HR 1.09, 95% CI 1.03ŌĆō1.15). |
| Nationwide Korean health screening database | Both MAFLD and NAFLD=2,625,321 | |
| MAFLD only=948,323 | ||
| NAFLD only=54,896 | ||
| Guerreiro et al. [52] (2021) | Total/MAFLD/NAFLD=171/154/109 | 1. Non-significant higher prevalence of high-risk cardiovascular scores was observed in MAFLD group compared to NAFLD group (36.4% vs. 25.7%, P=0.209). |
| Database of Brazillian patients undergoing liver biopsy at university hospital | Both MAFLD and NAFLD | |
| MAFLD only | ||
| NAFLD only |
Table┬Ā3.
Open research questions
Abbreviations
MAFLD
metabolic dysfunction-associated fatty liver disease
NAFLD
nonalcoholic fatty liver disease
NASH
non-alcoholic steatohepatitis
ALRD
alcohol-related liver disease
BMI
body mass index
NHANES
National Health and Nutrition Examination Surveys
FIB-4
fibrosis-4
FLD
fatty liver disease
CKD
chronic kidney disease
FEV1
forced expiratory volume in 1 second
REFERENCES
1. Ludwig J, Viggiano TR, McGill DB, Oh BJ. Nonalcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease. Mayo Clin Proc 1980;55:434-438.

2. Bellentani S. The epidemiology of non-alcoholic fatty liver disease. Liver Int 2017;37 Suppl 1:81-84.



3. Demirtas CO, Yilmaz Y. Metabolic-associated fatty liver disease: Time to integrate ground-breaking new terminology to our clinical practice? Hepatol Forum 2020;1:79-81.


4. Eslam M, Newsome PN, Sarin SK, Anstee QM, Targher G, Romero-Gomez M, et al. A new definition for metabolic dysfunctionassociated fatty liver disease: An international expert consensus statement. J Hepatol 2020;73:202-209.


5. Targher G, Tilg H, Byrne CD. Non-alcoholic fatty liver disease: a multisystem disease requiring a multidisciplinary and holistic approach. Lancet Gastroenterol Hepatol 2021;6:578-588.


6. El-Shabrawi M, Memon I, Attia D, El-Koofy NM. The International Society of Tropical Paediatrics (ISTP) endorses the redefinition of fatty liver disease. J Hepatol 2022;76:738-739.


7. Eslam M, Sarin SK, Wong VW, Fan JG, Kawaguchi T, Ahn SH, et al. The Asian Pacific Association for the Study of the Liver clinical practice guidelines for the diagnosis and management of metabolic associated fatty liver disease. Hepatol Int 2020;14:889-919.



8. Mendez-Sanchez N, Arrese M, Gadano A, Oliveira CP, Fassio E, Arab JP, et al. The Latin American Association for the Study of the Liver (ALEH) position statement on the redefinition of fatty liver disease. Lancet Gastroenterol Hepatol 2021;6:65-72.


9. Nan Y, An J, Bao J, Chen H, Chen Y, Ding H, et al. The Chinese Society of Hepatology position statement on the redefinition of fatty liver disease. J Hepatol 2021;75:454-461.


10. Shaltout I, Alkandari H, Fouad Y, Hamed AE. Arabic Association for the Study of Diabetes and Metabolism (AASD) endorsing the MAFLD definition of fatty liver disease. J Hepatol 2022;76:739-740.


11. Chalasani N, Younossi Z, Lavine JE, Charlton M, Cusi K, Rinella M, et al. The diagnosis and management of nonalcoholic fatty liver disease: Practice guidance from the American Association for the Study of Liver Diseases. Hepatology 2018;67:328-357.



12. Kawaguchi T, Tsutsumi T, Nakano D, Eslam M, George J, Torimura T. MAFLD enhances clinical practice for liver disease in the Asia-Pacific region. Clin Mol Hepatol 2022;28:150-163.




13. Wang X, Xie Q. Metabolic Dysfunction-associated Fatty Liver Disease (MAFLD) and Viral Hepatitis. J Clin Transl Hepatol 2022;10:128-133.

14. Younossi ZM, Paik JM, Al Shabeeb R, Golabi P, Younossi I, Henry L. Are there outcome differences between NAFLD and metabolicassociated fatty liver disease? Hepatology 2022;76:1423-1437.



15. Alexander M, Loomis AK, Fairburn-Beech J, van der Lei J, Duarte-Salles T, Prieto-Alhambra D, et al. Real-world data reveal a diagnostic gap in non-alcoholic fatty liver disease. BMC Med 2018;16:130.



16. Shiha G, Korenjak M, Eskridge W, Casanovas T, Velez-Moller P, H├Čgstr├Čm S, et al. Redefining fatty liver disease: an international patient perspective. Lancet Gastroenterol Hepatol 2021;6:73-79.


17. Nascimbeni F, Pais R, Bellentani S, Day CP, Ratziu V, Loria P, et al. From NAFLD in clinical practice to answers from guidelines. J Hepatol 2013;59:859-871.


18. Alem SA, Gaber Y, Abdalla M, Said E, Fouad Y. Capturing patient experience: A qualitative study of change from NAFLD to MAFLD real-time feedback. J Hepatol 2021;74:1261-1262.


19. Clayton M, Fabrellas N, Luo J, Alghamdi MG, Hafez A, Qadiri TA, et al. From NAFLD to MAFLD: Nurse and allied health perspective. Liver Int 2021;41:683-691.



20. Lim GEH, Tang A, Ng CH, Chin YH, Lim WH, Tan DJH, et al. An observational data meta-analysis on the differences in prevalence and risk factors between MAFLD vs NAFLD. Clin Gastroenterol Hepatol 2021 Dec 4;doi: 10.1016/j.cgh.2021.11.038.


21. Yamamura S, Eslam M, Kawaguchi T, Tsutsumi T, Nakano D, Yoshinaga S, et al. MAFLD identifies patients with significant hepatic fibrosis better than NAFLD. Liver Int 2020;40:3018-3030.



22. Zeng J, Qin L, Jin Q, Yang RX, Ning G, Su Q, et al. Prevalence and characteristics of MAFLD in Chinese adults aged 40 years or older: A community-based study. Hepatobiliary Pancreat Dis Int 2022;21:154-161.


23. Zhang YC, Lyu ZY, Ma B, Li LM, Wang W, Sheng C, et al. A new risk stratification strategy for fatty liver disease by incorporating MAFLD and fibrosis score in a large US population. Hepatol Int 2022;16:835-845.



24. Lazarus JV, , Mark HE, Anstee QM, Arab JP, Batterham RL, Castera L, et al.; NAFLD Consensus Consortium. Advancing the global public health agenda for NAFLD: a consensus statement. Nat Rev Gastroenterol Hepatol 2022;19:60-78.

25. Bergqvist CJ, Skoien R, Horsfall L, Clouston AD, Jonsson JR, Powell EE. Awareness and opinions of non-alcoholic fatty liver disease by hospital specialists. Intern Med J 2013;43:247-253.


26. Grant BF. Barriers to alcoholism treatment: reasons for not seeking treatment in a general population sample. J Stud Alcohol 1997;58:365-371.


27. Staufer K, Huber-Sch├Čnauer U, Strebinger G, Pimingstorfer P, Suesse S, Scherzer TM, et al. Ethyl glucuronide in hair detects a high rate of harmful alcohol consumption in presumed nonalcoholic fatty liver disease. J Hepatol 2022;77:918-930.


28. Meijnikman AS, Davids M, Herrema H, Aydin O, Tremaroli V, Rios-Morales M, et al. Microbiome-derived ethanol in nonalcoholic fatty liver disease. Nat Med 2022;28:2100-2106.



29. European Association for the Study of the Liver. EASL Clinical Practice Guidelines: Management of alcohol-related liver disease. J Hepatol 2018;69:154-181.


30. European Association for the Study of the Liver (EASL); European Association for the Study of Diabetes (EASD); European Association for the Study of Obesity (EASO). EASL-EASD-EASO clinical practice guidelines for the management of non-alcoholic fatty liver disease. Obes Facts 2016;9:65-90.




31. Lin S, Huang J, Wang M, Kumar R, Liu Y, Liu S, et al. Comparison of MAFLD and NAFLD diagnostic criteria in real world. Liver Int 2020;40:2082-2089.



32. Kang SH, Cho Y, Jeong SW, Kim SU, Lee JW; Korean NAFLD Study Group. From nonalcoholic fatty liver disease to metabolic-associated fatty liver disease: Big wave or ripple? Clin Mol Hepatol 2021;27:257-269.




33. Yu C, Wang M, Zheng S, Xia M, Yang H, Zhang D, et al. Comparing the diagnostic criteria of MAFLD and NAFLD in the chinese population: A population-based prospective cohort study. J Clin Transl Hepatol 2022;10:6-16.



34. Wieland AC, Mettler P, McDermott MT, Crane LA, Cicutto LC, Bambha KM. Low awareness of nonalcoholic fatty liver disease among patients at high metabolic risk. J Clin Gastroenterol 2015;49:e6-e10.


35. Cleveland ER, Ning H, Vos MB, Lewis CE, Rinella ME, Carr JJ, et al. Low awareness of nonalcoholic fatty liver disease in a population-based cohort sample: the CARDIA study. J Gen Intern Med 2019;34:2772-2778.




36. Kawaguchi T, Tsutsumi T, Nakano D, Torimura T. MAFLD: Renovation of clinical practice and disease awareness of fatty liver. Hepatol Res 2022;52:422-432.



37. Singh A, Dhaliwal AS, Singh S, Kumar A, Lopez R, Gupta M, et al. Awareness of nonalcoholic fatty liver disease is increasing but remains very low in a representative US cohort. Dig Dis Sci 2020;65:978-986.



38. Tharwat M, Medhat MA, El-Kassas M. The NAFLD-MAFLD debate through the lens of the Arab world. Saudi J Gastroenterol 2022;28:413-416.



39. Ayada I, van Kleef LA, Alferink LJM, Li P, de Knegt RJ, Pan Q. Systematically comparing epidemiological and clinical features of MAFLD and NAFLD by meta-analysis: Focusing on the nonoverlap groups. Liver Int 2022;42:277-287.



40. Baratta F, Ferro D, Pastori D, Colantoni A, Cocomello N, Coronati M, et al. Open issues in the transition from NAFLD to MAFLD: The experience of the plinio study. Int J Environ Res Public Health 2021;18:8993.



41. Kemp W, Clayton-Chubb D, Majeed A, Glenister KM, Magliano DJ, Lubel J, et al. Impact of renaming NAFLD to MAFLD in an Australian regional cohort: Results from a prospective population-based study. J Gastroenterol Hepatol 2022;37:395-403.



42. Sinn DH, Kang D, Choi SC, Hong YS, Zhao D, Guallar E, et al. Nonalcoholic fatty liver disease without metabolic-associated fatty liver disease and the risk of metabolic syndrome. Clin Gastroenterol Hepatol 2022 Sep 22;doi: 10.1016/j.cgh.2022.09.014.


43. Tang A, Ng CH, Phang PH, Chan KE, Chin YH, Fu CE, et al. Comparative burden of metabolic dysfunction in Lean NAFLD vs Non-lean NAFLD - A systematic review and metaanalysis. Clin Gastroenterol Hepatol 2022 Jul 19;doi: 10.1016/j.cgh.2022.06.029.


44. Moon JH, Kim W, Koo BK, Cho NH NH; Innovative Target Exploration of NAFLD (ITEN) consortium. Metabolic dysfunction-associated fatty liver disease predicts long-term mortality and cardiovascular disease. Gut Liver 2022;16:433-442.



45. Huang Q, Zou X, Wen X, Zhou X, Ji L. NAFLD or MAFLD: Which has closer association with all-cause and cause-specific mortality?-Results from NHANES III. Front Med (Lausanne) 2021;8:693507.



46. Muthiah M, Ng CH, Chan KE, Fu CE, Lim WH, Tan DJH, et al. Type 2 diabetes mellitus in metabolic-associated fatty liver disease vs. type 2 diabetes mellitus Non-alcoholic fatty liver disease: A longitudinal cohort analysis. Ann Hepatol 2022;28:100762.


47. Nguyen VH, Le MH, Cheung RC, Nguyen MH. Differential clinical characteristics and mortality outcomes in persons with NAFLD and/or MAFLD. Clin Gastroenterol Hepatol 2021;19:2172-2181 e6.


48. Semmler G, Wernly S, Bachmayer S, Leitner I, Wernly B, Egger M, et al. Metabolic Dysfunction-Associated Fatty Liver Disease (MAFLD)-Rather a Bystander Than a Driver of Mortality. J Clin Endocrinol Metab 2021;106:2670-2677.



49. Klein S, Gastaldelli A, Yki-J├żrvinen H, Scherer PE. Why does obesity cause diabetes? Cell Metab 2022;34:11-20.



50. Miyake T, Matsuura B, Furukawa S, Ishihara T, Yoshida O, Miyazaki M, et al. Fatty liver with metabolic disorder, such as metabolic dysfunction-associated fatty liver disease, indicates high risk for developing diabetes mellitus. J Diabetes Investig 2022;13:1245-1252.




51. Niriella MA, Ediriweera DS, Kasturiratne A, De Silva ST, Dassanayaka AS, De Silva AP, et al. Outcomes of NAFLD and MAFLD: Results from a community-based, prospective cohort study. PLoS One 2021;16:e0245762.



52. Guerreiro GTS, Longo L, Fonseca MA, de Souza VEG, Álvares-daSilva MR. Does the risk of cardiovascular events differ between biopsy-proven NAFLD and MAFLD? Hepatol Int 2021;15:380-391.



53. Lee H, Lee YH, Kim SU, Kim HC. Metabolic dysfunction-associated fatty liver disease and incident cardiovascular disease risk: A nationwide cohort study. Clin Gastroenterol Hepatol 2021;19:2138-2147 e10.


54. Bessho R, Kashiwagi K, Ikura A, Yamataka K, Inaishi J, Takaishi H, et al. A significant risk of metabolic dysfunction-associated fatty liver disease plus diabetes on subclinical atherosclerosis. PLoS One 2022;17:e0269265.



55. Sun DQ, Jin Y, Wang TY, Zheng KI, Rios RS, Zhang HY, et al. MAFLD and risk of CKD. Metabolism 2021;115:154433.


56. Miao L, Yang L, Guo LS, Shi QQ, Zhou TF, Chen Y, et al. Metabolic dysfunction-associated fatty liver disease is associated with greater impairment of lung function than nonalcoholic fatty liver disease. J Clin Transl Hepatol 2022;10:230-237.



57. Xue J, Wang QX, Xiao HM, Shi MJ, Xie YB, Li S, et al. Impact of metabolic dysfunction associated fatty liver disease on the prognosis of patients with Hepatitis B Virus-related hepatocellular carcinoma based on propensity score matching analysis. Cancer Manag Res 2022;14:2193-2202.




58. Zheng KI, Sun DQ, Jin Y, Zhu PW, Zheng MH. Clinical utility of the MAFLD definition. J Hepatol 2021;74:989-991.


59. Paternostro R, Trauner M. Current treatment of non-alcoholic fatty liver disease. J Intern Med 2022;292:190-204.




60. Ng CH, Huang DQ, Nguyen MH. Nonalcoholic fatty liver disease versus metabolic-associated fatty liver disease: Prevalence, outcomes and implications of a change in name. Clin Mol Hepatol 2022;28:790-801.




-
METRICS

- ORCID iDs
-
Cameron Gofton

https://orcid.org/0000-0002-0913-7180 - Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



