| Clin Mol Hepatol > Volume 28(3); 2022 > Article |
|
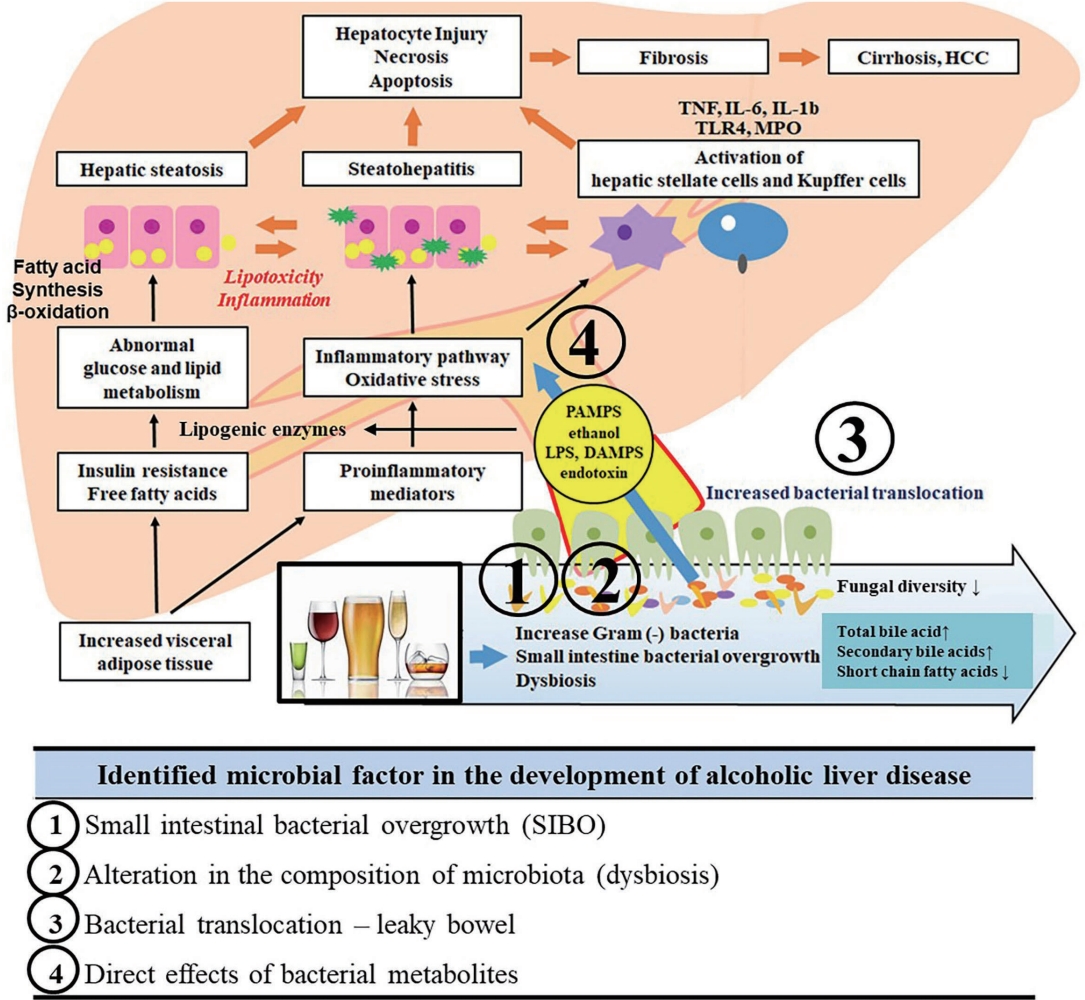
The gastrointestinal microbiome and metabolomics are the candidate biomarkers for alcoholic liver disease (ALD) [1]. Alcohol-associated liver injury is characterized by oxidative stress, lipid peroxidation, steatosis, iron deposits, hepatocyte damage, and hepatocytes death. These features have been associated with liver inflammation, activation of Kupffer cells and hepatic stellate cells, liver fibrosis, and liver regeneration process. Alcohol use promotes a change in microbiome composition. Microbiota-host co-regulated metabolic pathways are promising targets for clinical needs.
Metabolite profiles such as lipids, fatty acids, carbohydrates, vitamins, proteins, enzymatic compounds, amino acids, and small-molecules profoundly affected host physiology and are being explored for their roles in ALD. The molecular families are shaped by the microbiome with short-chain fatty acids (SCFA; acetate, propionate, and butyrate), aromatic amino acid metabolites, indoles, complex polysaccharides, and host lipids such as sphingolipids and bile acids [2,3]. SCFA were found in human large intestine and involved in microbial fermentation. SCFA play intestinal homeostasis and potent immune regulators. SCFA indicate that gut-brain-liver axis could impaired by alcohol [4,5].
Acetaldehyde is mainly expressed in hepatocytes and acts on hepatic stellate cells (HSCs) in a paracrine manner. Acetaldehyde directly increases expression of collagen-I in HSCs through transcription factors. Acetaldehyde reacts with metabolic components, which help maintain HSC activation. Ethanol increases fatty liver acid synthesis in hepatocytes via sterol regulatory element-binding protein-1c by increasing expression of lipogenic genes [6]. Interleukin (IL)-22 might be used treat to ALD patients because of its antioxidant, anti-apoptotic, anti-steatotic, anti-proliferative, and anti-microbial effects. Corticosteroids increased survival in patients with alcoholic hepatitis.
CXC chemokines such as CXCL12, CXCR4, and vascular endothelial growth factor have increased survival and the degree of hypertension. IL-8 and growth-related oncogene-alpha are parts of CXC chemokines family. These might be industrialized as a therapeutic drug for ALD [7].
Anti-tumor necrosis factor (TNF)-╬▒ has an important role in the pathogenies of ALD in animal models. Pentoxifylline blocks transcription of TNF-╬▒ which can decrease serum level of TNF-╬▒. S-adenosylmethionine (SAMe) acts as a methyl donor that has protect against ALD through antioxidant functions, and down regulation of TNF-╬▒. SAMe plays as a safe drug for ALD. However, Cochrane report indicated that there have no evidences to support the use of SAMe in ALD patients [8].
The time has come to develop the therapeutic biomarkers via gut-microbiome and metabolome in ALD. Patients with ALD show gut barrier dysfunction. Now, gut-microbiome-centered therapies are novel and associated metabolomics signature that plays a big platform for biomarkers discovery in ALD.
ACKNOWLEDGMENTS
This research was funded by Hallym University Research Fund, and the Basic Science Research Program through the National Research Foundation of Korea funded by the Ministry of Education, Science and Technology (NRF-2018M3A9F3020956, NRF-2019R1I1A3A01060447, NRF-2020R1I1A3073530 and NRF2020R1A6A1A03043026).
FOOTNOTES
REFERENCES
1. GBD 2016 Alcohol Collaborators. Alcohol use and burden for 195 countries and territories, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet 2018;392:1015-1035.


2. Hoyles L, Fern├Īndez-Real JM, Federici M, Serino M, Abbott J, Charpentier J, et al. Molecular phenomics and metagenomics of hepatic steatosis in non-diabetic obese women. Nat Med 2018;24:1070-1080.




3. Raja G, Gupta H, Gebru YA, Youn GS, Choi YR, Kim HS, et al. Recent advances of microbiome-associated metabolomics profiling in liver disease: principles, mechanisms, and applications. Int J Mol Sci 2021;22:1160.



4. Koh A, De Vadder F, Kovatcheva-Datchary P, B├żckhed F. From dietary fiber to host physiology: short-chain fatty acids as key bacterial metabolites. Cell 2016;165:1332-1345.


5. Mitchell RW, On NH, Del Bigio MR, Miller DW, Hatch GM. Fatty acid transport protein expression in human brain and potential role in fatty acid transport across human brain microvessel endothelial cells. J Neurochem 2011;117:735-746.


6. Mello T, Ceni E, Surrenti C, Galli A. Alcohol induced hepatic fibrosis: role of acetaldehyde. Mol Aspects Med 2008;29:17-21.


- TOOLS
-
METRICS

- ORCID iDs
-
Ki Tae Suk

https://orcid.org/0000-0002-9206-9245 - Related articles
-
Recent updates on pharmacologic therapy in non-alcoholic fatty liver disease2024 January;30(1)
Letter regarding ŌĆ£Risk factors in nonalcoholic fatty liver diseaseŌĆØ2023 October;29(4)
The effect of moderate alcohol consumption on nonalcoholic fatty liver disease2023 April;29(2)
Implications of comorbidities in nonalcoholic fatty liver disease2023 April;29(2)



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



