| Clin Mol Hepatol > Volume 29(4); 2023 > Article |
|
ABSTRACT
Background/Aims
Methods
Results
ACKNOWLEDGMENTS
FOOTNOTES
Supplementary materials
Supplementary Figure 1.
Supplementary Figure 2.
Supplementary Figure 3.
Supplementary Figure 4.
Supplementary Figure 5.
Supplementary Table 2.
Supplementary Table 3.
Supplementary Table 4.
Figure 1.

Figure 2.
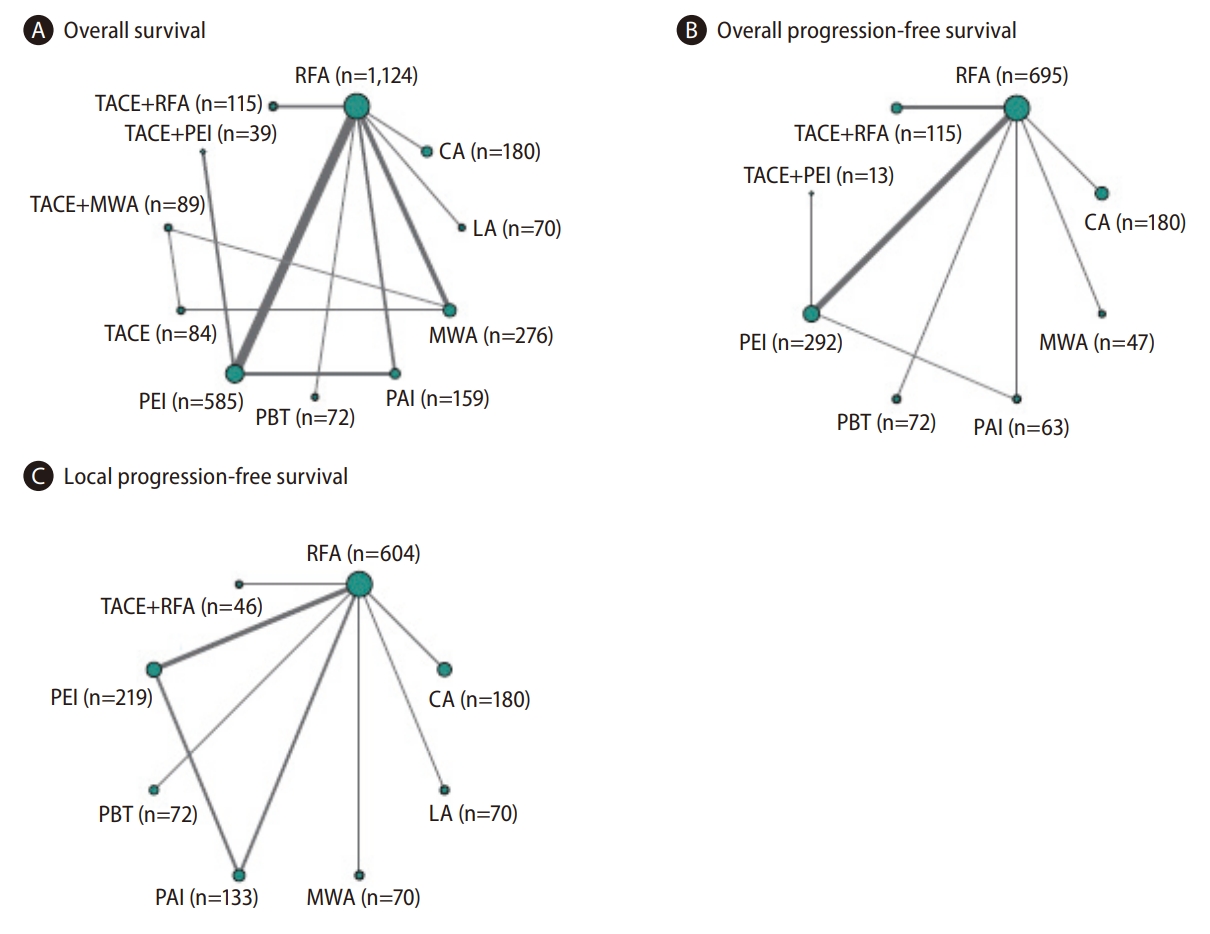
Figure 4.

Figure 5.
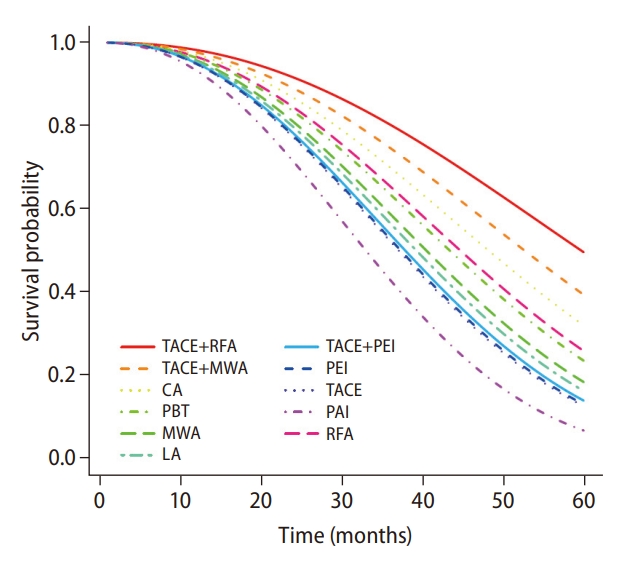
Figure 6.

Table 1.
| Study name (Country) | Arm | No. of patients | Inclusion criteria for tumor | Main tumor size* (cm) | Single HCC (%) | HCC ≤3 cm (%) | Male sex (%) | Age* (years) | Follow-up duration† (months) | CTP class A/B/C (%) | Outcome | Major complications‡ (%) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Abdelaziz et al. [23] 2014 (Egypt) | RFA | 45 | All <5 cm, number ≤3 | 2.95 | 86.7 | 61.5 | 68.9 | 56.8 | 27 | 53.3/46.7/- | OS | ND |
| MWA | 66 | 2.90 | 86.4 | 72.4 | 72.7 | 53.6 | 27 | 37.9/62.1/- | ND | |||
| Brunello et al. [24] 2008 (Italy) | PEI | 69 | All ≤3 cm, number ≤3 | 2.25 | 78.7 | 100 | 71.0 | 70.3 | 26 | 56.5/43.5/- | OS | 2.9 |
| RFA | 70 | 2.42 | 77.1 | 100 | 61.4 | 69 | 25 | 54.3/45.7/- | 2.9 | |||
| Chong et al. [25] 2020 (Hong Kong) | MWA | 47 | All ≤5 cm, number ≤3 | Median, 3.1 | 91.5 | 51.1 | 63.8 | Median, 63 | 38.3 | 83.0/14.9/2.1 | OS, overall PFS | ND |
| RFA | 46 | Median, 2.8 | 84.8 | 32.6 | 82.6 | Median, 64.5 | 34 | 87.0/13.0/- | ND | |||
| Di Costanzo et al. [26] 2015 (Italy) | RFA | 70 | Within Milan criteria | 2.55 | 90.0 | 90.0 | 75.7 | Median, 70 | Mean, 42.8 | 90.0/10.0/- | OS, local PFS | 1.4 |
| LA | 70 | 2.62 | 87.1 | 78.6 | 67.1 | Median, 70 | Mean, 42.2 | 95.7/4.3/- | 1.4 | |||
| Giorgio et al. [27] 2011 (Italy) | PEI | 143 | Single ≤3 cm | 2.27 | 100 | 100 | 71.3 | 72 | 37 | 52.4/47.6/- | OS | ND |
| RFA | 142 | 2.34 | 100 | 100 | 73.9 | 70 | 37 | 49.3/50.7/- | ND | |||
| Kim et al. [8] 2021 (South Korea) | PBT | 72 | All <3 cm, number ≤2 | Median, 1.2 | 93.1 | 100 | 84.7 | Median, 60 | 51.6 | 97.2/2.8/- | OS, overall PFS, local PFS | 0 |
| RFA | 72 | Median, 1.2 | 91.7 | 100 | 81.9 | Median, 61.5 | 50.8 | 97.2/2.8/- | 1.4 | |||
| Koda et al. [36] 2001 (Japan) | TACE+PEI | 26 | All <3 cm, number ≤3 | 2.0 | 61.5 | 100 | 53.8 | 66.2 | 29 | 73.1/19.2/7.7 | OS | 7.7 |
| PEI | 26 | 1.9 | 57.7 | 100 | 69.2 | 66.4 | 31.2 | 53.8/30.8/15.4 | 0 | |||
| Lencioni et al. [6] 2003 (Italy) | RFA | 52 | Within Milan criteria | 2.8 | 76.9 | 88.5 | 69.2 | 67 | 22.9 | 86.5/13.5/- | OS, overall PFS, local PFS | 0 |
| PEI | 50 | 2.8 | 62.0 | 84.0 | 60.0 | 69 | 22.4 | 70.0/30.0/- | 0 | |||
| Lin et al. [28] 2004 (Taiwan) | RFA | 52 | All 1-4 cm, number ≤3 | 2.9 | 73.1 | 71.2 | 67.3 | 62 | 24.5 | 78.8/21.2/- | OS, overall PFS, local PFS | 0 |
| PEI | 52 | 2.8 | 76.9 | 73.1 | 65.4 | 59 | 23.8 | 75.0/25.0/- | 0 | |||
| Lin et al. [29] 2005 (Taiwan) | RFA | 62 | All ≤3 cm, number ≤3 | 2.5 | 79.0 | 100 | 64.5 | 61 | 28 | 74.2/25.8/- | OS, overall PFS, local PFS | 4.8 |
| PEI | 62 | 2.3 | 79.0 | 100 | 62.9 | 60 | 26 | 75.8/24.2/- | 0 | |||
| PAI | 63 | 2.3 | 76.2 | 100 | 66.7 | 63 | 26 | 71.4/28.6/- | 0 | |||
| Mizuki et al. [37] 2010 (Japan) | PEI | 14 | All 2-4 cm, number ≤3 | 2.64 | 78.6 | ND | 50.0 | 63.6 | 33 | ND | OS, overall PFS | 0 |
| TACE+PEI | 13 | 2.64 | 61.5 | ND | 69.2 | 65.8 | 39.7 | ND | 0 | |||
| Paul et al. [30] 2020 (India) | PAI | 26 | All ≤5 cm, number ≤ 5 | 2.7 | 80.8 | 66.7 | 76.9 | 53.5 | 13 | 73.1/26.9/- | OS | 7.7 |
| RFA | 29 | 2.7 | 89.7 | 57.6 | 69.0 | 54.5 | 15 | 62.1/37.9/- | 6.9 | |||
| Peng et al. [31] 2012 (China) | TACE+RFA | 69 | Within Milan criteria | 2.1 | 94.2 | 59.4 | 85.5 | 57.5 | 39.2 | 87.0/13.0/- | OS, overall PFS | 2.9 |
| RFA | 70 | 2.1 | 92.9 | 65.7 | 78.6 | 55.1 | 33.6 | 84.3/15.7/- | 2.9 | |||
| Shibata et al. [32] 2009 (Japan) | TACE+RFA | 46 | All ≤3 cm, number ≤3 | 1.7 | ND | 100 | 67.4 | 67.2 | 30.4 | 69.6/30.4/- | OS, overall PFS, local PFS | 2.2 |
| RFA | 43 | 1.6 | ND | 100 | 76.7 | 69.8 | 30.4 | 76.7/23.3/- | 2.3 | |||
| Shiina et al. [33] 2005 (Japan) | RFA | 118 | All ≤3 cm, number ≤3 | ND | 61.0 | 100 | 66.9 | ≤65/>65, n=44/74 | 37.2 | 72.0/28.0/- | OS, overall PFS | 3.4 |
| PEI | 114 | ND | 52.6 | 100 | 76.3 | ≤65/>65, n=41/73 | 34.8 | 74.6/25.4/- | 2.6 | |||
| Tsai et al. [38] 2008 (Taiwan) | PAI | 70 | All ≤4 cm, number ≤3 | 2.2 | 84.3 | ND | 67.1 | 65 | Mean, 43 | 80.0/20.0/- | OS, local PFS | 1.4 |
| PEI | 55 | 2.2 | 85.5 | ND | 74.5 | 66 | Mean, 43 | 70.9/29.1/- | 0 | |||
| Vietti Violi et al. [34] 2018 (France and Switzerland) | MWA | 70 | All ≤4 cm, number ≤3 | 1.8 | 62.0 | ND | 83.1 | Median, 68 | 26 | 80.3/19.7/- | OS, local PFS | 2.8 |
| RFA | 73 | 1.8 | 63.0 | ND | 84.9 | Median, 65 | 25 | 72.6/27.4/- | 4.1 | |||
| Wang et al. [10] 2015 (China) | CA | 180 | All ≤4 cm, number ≤2 | ND | 89.4 | ND | 77.8 | 53.9 | 25 | 67.2/32.8/- | OS, overall PFS, local PFS | 3.9 |
| RFA | 180 | ND | 95.0 | ND | 83.3 | 53.3 | 25 | 60.6/39.4/- | 3.3 | |||
| Zaitoun et al. [35] 2021 (Egypt) | TACE | 84 | Single 3-5 cm | 3.6 | 100 | ND | 61.9 | 51.3 | Mean, 19 | 84.5/15.5/- | OS | 3.6 |
| MWA | 92 | 3.9 | 100 | ND | 54.3 | 53.8 | Mean, 21 | 84.8/15.2/- | 2.2 | |||
| TACE+MWA | 89 | 3.7 | 100 | ND | 58.4 | 52.1 | Mean, 24 | 89.9/10.1/- | 1.1 |
HCC, hepatocellular carcinoma; CTP, Child-Turcotte-Pugh; RFA, radiofrequency ablation; MWA, microwave ablation; PEI, percutaneous ethanol injection; LA, laser ablation; TACE, transarterial chemoembolization; PBT, proton beam therapy; PAI, percutaneous acetic acid injections; CA, cryoablation; OS, overall survival; PFS, progression-free survival; ND, not described in the text.
‡ Results for major complications were based on the criteria defined and set by the individual studies: (for example) bowel perforation, hemorrhage, infection, third space fluid collection needing intervention, pneumothorax needing chest tube, needle-track tumor seeding, hepatic failure, and procedure-related death.
Abbreviations
REFERENCES
- TOOLS
-
METRICS

- ORCID iDs
-
Seungbong Han

https://orcid.org/0000-0003-2938-8072Ju Hyun Shim

https://orcid.org/0000-0002-7336-1371 - Related articles




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Supplement1
Supplement1 Print
Print



